Services
TREATMENT
Treatment for cancer can involve Surgery, Radiation, Chemotherapy as well as other modalities. Vincere provides state of the art treatment as well as going further into next generation cancer care.
SURGERY
Vincere has surgical facilities that rival the best in the nation: from the Endoscopy suites to the class C operating rooms and hybrid room, and comforting recovery areas. However, even more important is our Operative and Recovery Nurses and Staff that truly put our patient’s needs above all else.
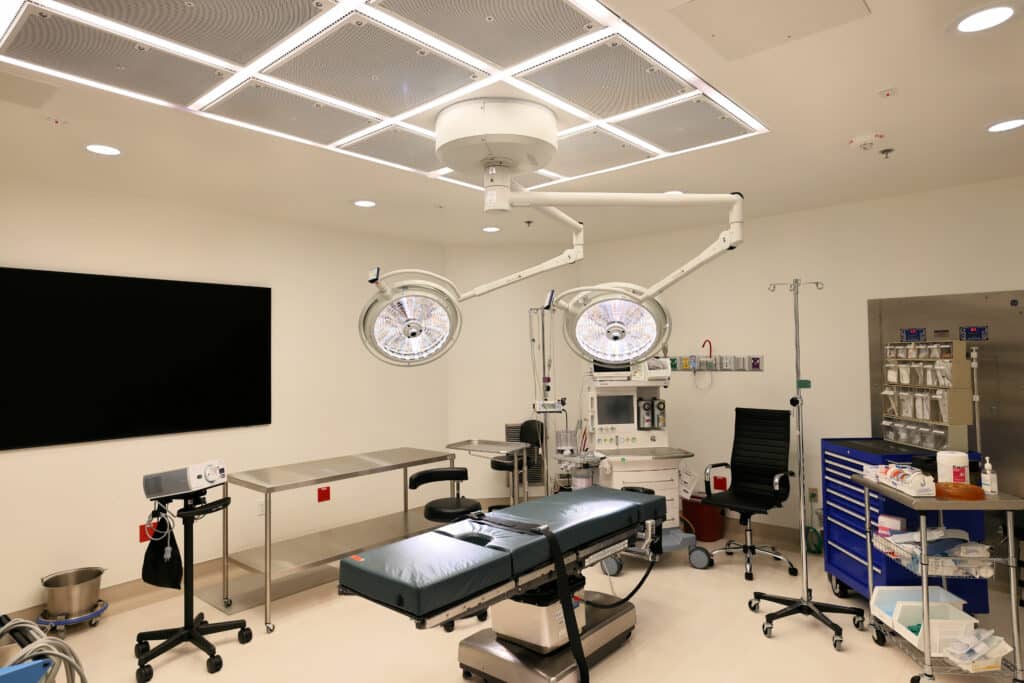


RADIATION THERAPY
Your Radiation Team is very important as you will be seeing them 5 days a week for multiple weeks, depending on your treatment plan as given by the Radiation Oncologist. The Vincere Radiation Team executes this plan with precision, but also in a caring manner and is a joy to work with. Everyone from the Radiation Technologists, Dosimetrist, PhD Physicists, and Receptionists, work diligently to implement the Radiation Plan. We are at the forefront of treatment plans, including IMRT, IGRT and hypofractionation, and tailor each plan to the patient, and their cancer. Protecting vital organs while targeting the tumor as precisely as possible gives the patient the greatest chance of cure while having the least morbidity.
VINCERE LABS
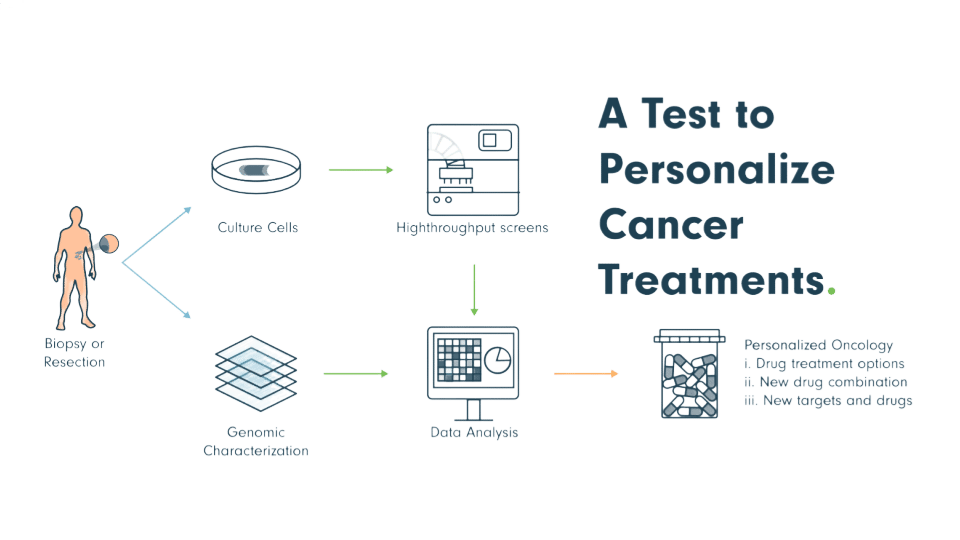
CHEMOTHERAPY/PRECISION MEDICINE
The genetics of cancer cells are as individual as the genetics of the patient. Two patients may have the same type and stage of cancer, yet react completely differently to the same treatment. Therefore it is important to fully understand the genomics of a particular cancer and patient and tailor the treatment; from surgery, radiation, chemotherapy, immunotherapy and other targeted therapies, to the individual patient to maximize the results and cure rates. This is also done to minimize the morbidity to the patient and offer them the least toxic therapy that will work on their specific genomics.
Standard Cancer Care takes a group of individuals with a specific cancer type/stage and averages the results in large studies based on different treatments. The next stage in Cancer Care Evolution is the ‘N of 1’ studies where a patient’s cancer cells are grown outside the body and these cells are treated with a library of chemotherapy, immunotherapy, and targeted therapy drugs, and the results (relative cancer cell kill rate) of the different drugs used to treat those cells outside the body are compared. Each patient’s cancer cells are then entered into its own ‘study’ and the cells are treated with up to 50 different treatments before the patient undergoes therapy in order to find the best drug for that patient’s treatment. This type of precision medicine testing, along with genomic sequencing of the tumor, can give a strong prediction as to whether or not a specific chemotherapy drug or other therapeutics will be effective against a specific patient’s tumor.





MOLECULAR RESIDUAL DISEASE (MRD)
Once Cancer free, it is important to closely monitor for any recurrence of disease. The standard way this is done is through periodic imaging such as CT-scans, or MRI. A new cutting edge method is used to detect the cancer recurrence on the molecular level. A small sample of your tumor along with a blood sample is used to make a customized test to each individual. Then periodically, just a blood sample, or ‘liquid biopsy’, is tested. This individualized MRD testing detects a recurrence on average 1 – 2 years before a recurrence can be seen on imaging. This allows for much sooner treatment if necessary while the recurrence is very small.
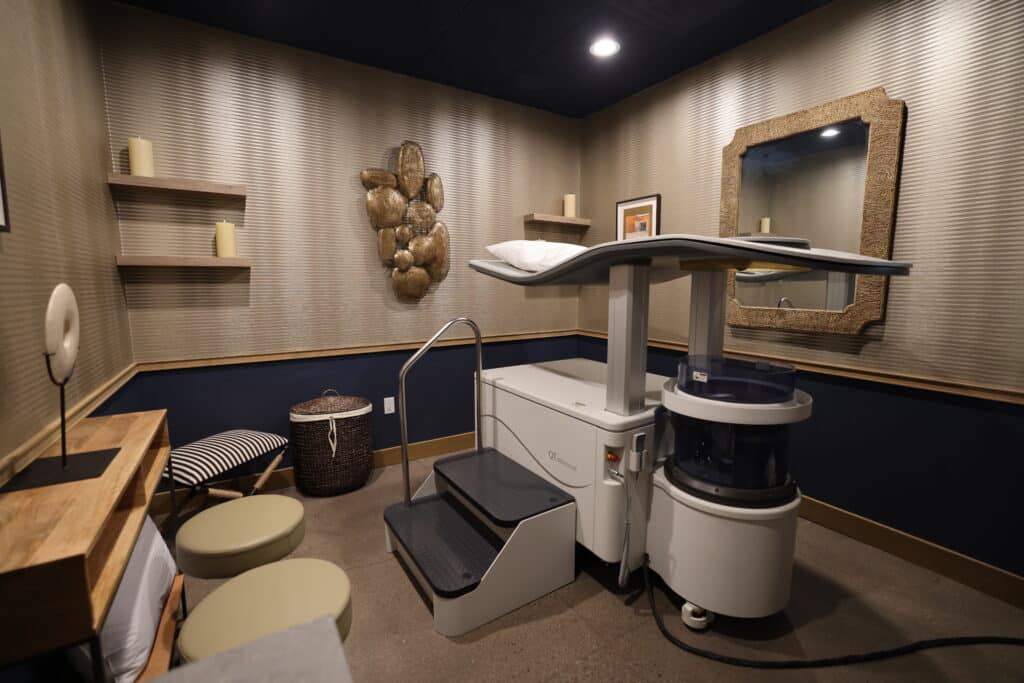
QUANTITATIVE TRANSMISSION ULTRASOUND
While there is no current replacement for traditional mammograms, QT Ultrasound offers a novel way of imaging the breast and is only 1 of 5 machines in the United States.
A mammogram is a very important tool in breast screening for cancer, but it also has its limitations. Breast cancer is sadly becoming more prevalent in younger women, and often is present before a mammogram can detect a mass.
The reason for this is that mammograms are best suited for women with breast tissue that is less dense. When breast tissue is dense, which is usually the case for women under 40, and some women over 40, it’s difficult for a radiologist to find a small mass causing distortion in a sea of white.
Traditional ultrasound is used in these patients to try to search for masses. Traditional ultrasound uses older Reflective Ultrasound technology, where the ultrasound waves bounce off of the breast tissue and back to the receiver which interprets the data. This results in an image that is only a small part of the whole.
With Transmission Ultrasound, the ultrasound waves travel through the breast tissue and the receiver is on the opposite side of the breast reading the data. This is performed in true 3D to form a more complete picture of the breast. The images resemble those of an MRI, and show detail down to the ductal level.
Another benefit of QT Ultrasound, is that it’s better at seeing around breast implants. Traditional mammograms can only see what is squeezed between the imaging plates. A breast implant can inhibit how much of the breast tissue is visualized. Since there is no squeezing in QT Ultrasound, the imaging sees the breast tissue that is placed in the water bath while the patient is laying down on her stomach.
Finally, QT Ultrasound does not use radiation for imaging as mammograms do.